Table of Contents
A Comprehensive Guide to Abdominal Pain, Causes, Symptoms, Diagnosis, and Treatment
Introduction: The Universal Signal
Abdominal pain is one of the most common reasons for visits to emergency rooms and primary care physicians worldwide. It is a universal human experience; almost everyone will experience a “stomach ache” at some point in their lives. However, the term “abdominal pain” is deceptively simple. The abdomen is a complex anatomical region housing a multitude of vital organs, including the stomach, liver, gallbladder, pancreas, small and large intestines, spleen, kidneys, and reproductive organs. Pain in this area can range from a mild, fleeting discomfort to a severe, life-threatening emergency.
Understanding abdominal pain requires more than just acknowledging a symptom; it requires decoding a signal. It is the body’s way of communicating that something within the complex ecosystem of the torso is amiss. Because the abdomen contains so many different structures, the location, intensity, and type of pain are crucial clues in determining the underlying cause. What feels like simple indigestion could be early signs of cardiac issues, while what feels like severe cramping might be a passing virus.
This comprehensive guide aims to demystify abdominal pain. We will explore the anatomy of discomfort, categorize the types of pain, delve into the myriad causes ranging from benign to critical, examine diagnostic protocols, and outline modern treatment strategies. By the end of this article, you will have a deeper understanding of what your body might be telling you when pain strikes your core.
The Anatomy of Discomfort: Location Matters
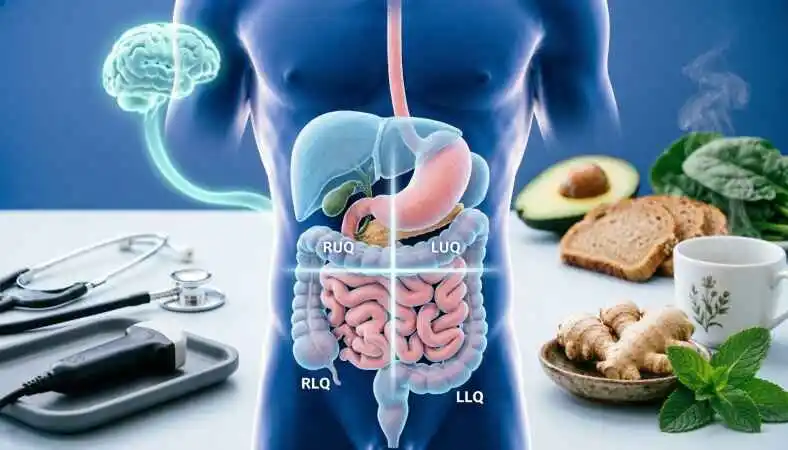
To understand abdominal pain, one must first understand the map of the abdomen. Physicians divide the abdomen into four quadrants to pinpoint the source of pain. This localization is the first step in diagnosis.
The Four Quadrants
- Right Upper Quadrant (RUQ): Houses the liver, gallbladder, right kidney, and parts of the pancreas and colon. Pain here is often associated with liver disease, gallstones, or hepatitis.
- Left Upper Quadrant (LUQ): Contains the stomach, spleen, left kidney, and parts of the pancreas and colon. Pain here might suggest gastritis, pancreatitis, or splenic issues.
- Right Lower Quadrant (RLQ): Home to the appendix, right ovary (in females), and parts of the colon. This is the classic site for appendicitis.
- Left Lower Quadrant (LLQ): Contains the left ovary (in females), sigmoid colon, and descending colon. Pain here is common in diverticulitis and kidney stones.
Epigastric and Hypogastric Regions
In addition to the quadrants, the central regions are vital.
- Epigastric Region (Upper Middle): Located just below the ribs. This is the “pit of the stomach.” Pain here is frequently related to the stomach, esophagus, or heart. Conditions like GERD, peptic ulcers, and even myocardial infarction (heart attack) often manifest here.
- Hypogastric/Suprapubic Region (Lower Middle): Located below the belly button. Pain here often involves the bladder, uterus (in females), or rectum. Urinary tract infections (UTIs) and menstrual cramps are common culprits here.
Understanding this map helps patients articulate their symptoms more effectively, allowing for faster and more accurate medical assessment.
Classifying the Types of Pain
Not all pain feels the same. The character of the pain is just as important as its location. Physicians categorize abdominal pain into three primary types based on how the nerves transmit the signal.
1. Visceral Pain
Visceral pain originates from the organs (viscera). The organs themselves have a lower density of pain receptors compared to the skin, and the pain is often difficult to localize.
- Characteristics: It is often described as a dull, aching, or gnawing sensation. It can feel like a deep pressure.
- Radiation: Because the nerves serving the organs share pathways with other areas, visceral pain often radiates to other parts of the body. For example, the pain of a heart attack often radiates to the left arm or jaw, and gallbladder pain often radiates to the right shoulder blade.
- Causes: Distension of an organ (stretching), inflammation, or ischemia (lack of blood flow).
2. Parietal (Somatic) Pain
Parietal pain originates from the parietal peritoneum, the lining of the abdominal cavity. This lining has a high density of nerve endings, making the pain sharp and precise.
- Characteristics: Patients can usually point to the exact spot of the pain with one finger. It is often severe, sharp, and aggravated by movement or coughing.
- Causes: This type of pain usually signals inflammation of the lining, such as in appendicitis or peritonitis (infection of the abdominal cavity).
3. Referred Pain
Referred pain is felt at a location distant from the source of the issue.
- Mechanism: This happens because nerve pathways from different parts of the body converge at the same level of the spinal cord. The brain misinterprets the signal location.
- Examples: Liver inflammation (gallbladder issues) causing pain in the right shoulder; a pelvic abscess causing pain in the rectum; or pneumonia causing pain in the upper abdomen due to irritation of the diaphragm.
Temporal Classification
- Acute Pain: Develops suddenly, often severely. It is usually a sign of a structural change requiring immediate attention (e.g., a burst appendix).
- Chronic Pain: Persists for weeks or months. It may be intermittent or constant and is often related to functional disorders (like IBS) or chronic inflammatory conditions (like Crohn’s disease).
Unraveling the Causes: From Mild to Severe
The causes of abdominal pain are vast. They can be categorized by the body system involved or the severity of the condition.
Gastrointestinal Causes
The digestive tract is the most common source of abdominal pain.
- Gastroenteritis (Stomach Flu): Caused by viral or bacterial infections. Symptoms include cramping, diarrhea, and vomiting. It is usually self-limiting but can cause dehydration.
- Gas and Bloating: Trapped gas in the digestive tract can cause sharp, stabbing pains that move location. It is extremely common and usually relieved by passing gas or belching.
- Gastritis and Peptic Ulcers: Inflammation of the stomach lining (gastritis) or sores in the stomach lining (ulcers) cause burning epigastric pain, often worsened by eating (in the case of gastric ulcers) or improved by eating (in the case of duodenal ulcers).
- Inflammatory Bowel Disease (IBD): Includes Crohn’s disease and ulcerative colitis. These are autoimmune conditions causing chronic inflammation, leading to severe pain, weight loss, and diarrhea.
- Irritable Bowel Syndrome (IBS): A functional disorder where the gut-brain interaction is disrupted. It causes cramping, bloating, and altered bowel habits without visible structural damage.
- Appendicitis: A medical emergency where the appendix becomes inflamed and filled with pus. Pain typically starts near the navel and migrates to the RLQ. It requires immediate surgical removal.
- Diverticulitis: Inflammation or infection of small pouches (diverticula) that form in the walls of the colon. This causes LLQ pain, fever, and nausea.
Hepatobiliary and Pancreatic Causes
- Gallstones (Cholelithiasis): Hardened deposits of digestive fluid in the gallbladder. They can block the bile ducts, causing intense RUQ pain (biliary colic), especially after fatty meals.
- Pancreatitis: Inflammation of the pancreas. It causes severe, upper abdominal pain that often radiates to the back. It is frequently caused by gallstones or heavy alcohol use.
Urinary and Renal Causes
- Kidney Stones: Mineral deposits that form in the kidneys. When they pass into the ureter, they cause excruciating waves of pain in the flank (side) that radiate to the lower abdomen and groin.
- Urinary Tract Infections (UTIs): Infections of the bladder or urethra causing lower abdominal pressure, burning during urination, and frequent urges to void.
Gynecological Causes (Female-Specific)
- Dysmenorrhea: Painful menstrual cramps caused by uterine contractions.
- Endometriosis: A condition where tissue similar to the uterine lining grows outside the uterus, causing chronic pelvic pain.
- Ovarian Cysts: Fluid-filled sacs on the ovaries. Rupture or torsion (twisting) of a cyst causes sudden, severe lower abdominal pain.
- Ectopic Pregnancy: A life-threatening condition where a fertilized egg implants outside the uterus (usually in the fallopian tube). It causes severe RLQ or LLQ pain and vaginal bleeding.
Systemic and Other Causes
- Food Intolerances: Lactose intolerance or Celiac disease can cause significant bloating, gas, and cramping after consuming trigger foods.
- Hernias: Occur when an organ pushes through an opening in the muscle or tissue that holds it in place. An incarcerated or strangulated hernia causes severe pain and is a surgical emergency.
- Abdominal Aortic Aneurysm (AAA): A weakening of the wall of the aorta, the major blood vessel supplying the body. A rupture causes severe, tearing pain in the back and abdomen and is fatal if not treated immediately.
Recognizing the Symptoms
While pain is the primary symptom, associated symptoms are critical for narrowing down the diagnosis.
Digestive Symptoms
- Nausea and Vomiting: Common in gastroenteritis, appendicitis, and pancreatitis. The presence of blood in vomit (hematemesis) indicates a serious issue, such as a bleeding ulcer or torn esophagus.
- Diarrhea or Constipation: Changes in bowel habits are hallmark signs of IBS, IBD, or infections. Bloody stools (hematochezia) suggest inflammation, infection, or cancer.
- Loss of Appetite (Anorexia): A very specific symptom of appendicitis; patients often report they “just don’t want to eat.”
Systemic Symptoms
- Fever: Indicates an infection, such as appendicitis, diverticulitis, or cholecystitis.
- Weight Loss: Unintentional weight loss with abdominal pain can be a red flag for malignancy or severe malabsorption issues like Celiac disease.
- Jaundice: Yellowing of the skin and eyes points to liver or gallbladder issues.
“Red Flag” Symptoms
Medical professionals use the term “red flags” to identify symptoms that suggest a serious or life-threatening condition. Immediate medical attention is required if abdominal pain is accompanied by:
- Rigid Abdomen: The stomach muscles are tight and board-like. This suggests peritonitis (infection of the abdominal lining).
- Rebound Tenderness: Pain is worse when pressure is released rather than applied.
- Hematemesis or Hematochezia: Vomiting blood or passing bloody/tarry stools.
- Syncope: Fainting or dizziness, which may indicate internal bleeding or severe dehydration.
- Dysphagia: Difficulty swallowing.
- Shortness of Breath: Can suggest a heart attack or severe infection.
The Diagnostic Journey
Diagnosing abdominal pain is often like detective work. Physicians use a combination of history, physical exams, and technology.
1. Clinical History (Anamnesis)
The doctor will ask specific questions using the “OPQRST” mnemonic:
- Onset: When did the pain start? Was it sudden or gradual?
- Provocation/Palliation: What makes it better or worse? (Eating, movement, breathing?)
- Quality: Is it sharp, dull, burning, or cramping?
- Radiation: Does the pain travel?
- Severity: On a scale of 1-10, how bad is it?
- Timing: Is it constant or does it come and go?
2. Physical Examination
- Inspection: Looking for distension, scars, or visible pulsations.
- Auscultation: Listening to bowel sounds with a stethoscope. Absent sounds suggest ileus (paralysis of the bowel), while hyperactive sounds suggest obstruction or diarrhea.
- Percussion: Tapping the abdomen to detect fluid, air, or organ enlargement.
- Palpation: Pressing on the abdomen to identify areas of tenderness, masses, or guarding (tensing of muscles to protect the underlying pain).
3. Laboratory Tests
- Complete Blood Count (CBC): Checks for anemia and infection (elevated White Blood Cells).
- Comprehensive Metabolic Panel (CMP): Evaluates liver and kidney function, electrolytes, and blood sugar. Elevated liver enzymes point to hepatitis or gallbladder disease; elevated creatinine points to kidney issues.
- Lipase/Amylase: Enzymes that spike during pancreatitis.
- Urinalysis: Detects blood, infection, or stones in the urinary tract.
- Pregnancy Test: Essential for any female of childbearing age with abdominal pain to rule out ectopic pregnancy.
4. Imaging Studies
Ultrasound: The first-line imaging for gallbladder issues, kidney stones, and gynecological problems. It uses sound waves and is safe for pregnancy.
- CT Scan (Computed Tomography): The gold standard for acute abdominal pain. It provides detailed cross-sectional images of bones, muscles, fat, and organs. It is excellent for diagnosing appendicitis, diverticulitis, and bowel obstructions.
- MRI (Magnetic Resonance Imaging): Less commonly used for acute pain due to time and cost, but excellent for soft tissue detail, particularly in liver and pancreatic issues.
- Endoscopy/Colonoscopy: Inserting a camera down the throat (EGD) or up the rectum (colonoscopy) to visualize the inner lining of the gut. This is used for diagnosing ulcers, polyps, and IBD.
Treatment Strategies
Treatment depends entirely on the diagnosis. Management ranges from lifestyle changes to emergency surgery.
Conservative and Medical Management
- Dietary Modification: For mild conditions like GERD, gastritis, or IBS, avoiding trigger foods (spicy, fatty, acidic) is the first step. A “bland diet” or low-FODMAP diet is often prescribed.
- Medications:
- Antacids/PPIs: Proton pump inhibitors (like Omeprazole) reduce stomach acid for ulcers and GERD.
- Antibiotics: Prescribed for bacterial infections like H. pylori (ulcers), diverticulitis, or UTIs.
- Antispasmodics: Drugs like dicyclomine help relax gut muscles for IBS cramps.
- Analgesics: Acetaminophen is generally safe for pain, but NSAIDs (Ibuprofen, Aspirin) should be avoided if gastritis or ulcers are suspected, as they can worsen bleeding. Opioids are used for severe pain (kidney stones, pancreatitis) under strict supervision.
- Hydration: Essential for gastroenteritis to replace fluids lost from vomiting and diarrhea.
Interventional Procedures
- Endoscopy: Can be used therapeutically to stop bleeding ulcers, remove polyps, or dilate narrowed areas of the esophagus.
- Paracentesis: Removing excess fluid from the abdomen (ascites) to relieve pressure and breathing difficulties, common in liver disease.
Surgical Management
Surgery is required for “surgical abdomens”—conditions where an organ has ruptured, blocked, or is decaying.
- Appendectomy: Removal of the appendix. This is often done laparoscopically (keyhole surgery), allowing for small incisions and faster recovery.
- Cholecystectomy: Removal of the gallbladder. It is a very common surgery, usually performed after the patient recovers from an acute attack of cholecystitis.
- Bowel Resection: Removing a damaged part of the intestine due to cancer, perforation, or severe Crohn’s disease.
- Hernia Repair: Pushing the protruding tissue back into place and reinforcing the abdominal wall with mesh.
Chronic Pain Management
For conditions like IBS or chronic pancreatitis, where a “cure” may not be surgically achievable, a multidisciplinary approach is needed. This includes pain management specialists, dietary counseling, and sometimes low-dose antidepressants (tricyclic antidepressants), which are effective at modulating nerve pain signals in the gut.
Prevention and Self-Care
While not all abdominal pain can be prevented, a gut-healthy lifestyle can reduce the risk of many common disorders.
- Hydration: Drinking plenty of water aids digestion and prevents constipation and kidney stones.
- Fiber Intake: A diet rich in fruits, vegetables, and whole grains keeps the digestive tract moving, preventing diverticulitis and constipation. However, fiber should be increased gradually to avoid gas and bloating.
- Mindful Eating: Eating slowly, chewing food thoroughly, and not overeating can reduce indigestion and heartburn.
- Regular Exercise: Physical activity helps stimulate the natural contractions of the intestines, reducing the risk of bloating and constipation.
- Limit Irritants: Reducing alcohol consumption (which irritates the stomach lining and pancreas) and quitting smoking (which contributes to ulcers and Crohn’s disease) are vital preventative measures.
- Food Safety: Properly washing hands and cooking food prevents parasitic and bacterial infections like Salmonella and E. coli.
When to Call the Doctor
It is often difficult for a layperson to distinguish between “bad gas” and “appendicitis.” A general rule of thumb is to seek medical attention if:
- The pain is severe enough to wake you from sleep.
- The pain lasts more than a few days or is progressively getting worse.
- You have a fever over 100.4°F (38°C).
- You cannot keep liquids down (risk of dehydration).
- Your abdomen is tender to the touch.
- You notice blood in your stool or vomit.
Abdominal Migraines
What is an Abdominal Migraine?
An abdominal migraine is a variant of migraine disease that manifests primarily as abdominal pain rather than a headache. It is a functional gastrointestinal disorder, meaning the structure of the digestive tract is normal, but the way it functions is impaired due to a neurological trigger. While it is most commonly diagnosed in children aged 5–9, it can occur in adults and is often underdiagnosed.
Symptoms and Characteristics. Unlike a standard stomach ache, abdominal migraines follow a specific pattern similar to cranial migraines:
- Location: The pain is usually located around the belly button (periumbilical) and is described as a dull or sore ache (though it can be severe).
- Duration: Episodes can last anywhere from 2 to 72 hours.
- Associated Symptoms: The hallmark symptoms include severe nausea, vomiting, extreme pallor (looking very pale), and loss of appetite.
- Absence of Headache: By definition, a headache is not the primary symptom, distinguishing it from a classic migraine, though children with abdominal migraines often develop standard migraines later in adolescence or adulthood.
Causes and Triggers The exact mechanism is not fully understood, but it involves changes in the levels of histamine and serotonin, as well as fluctuations in the interaction between the brain and the gut. Triggers are nearly identical to those of standard migraines:
- Stress or anxiety.
- Specific foods (chocolate, processed meats, cheese, citrus).
- Fasting or skipping meals.
- Bright lights or strong smells.
- Sleep deprivation.
Diagnosis: Diagnosing abdominal migraines is often a process of elimination. Doctors must first rule out structural causes like appendicitis, kidney disease, or IBD. A diagnosis is typically confirmed if the patient has had at least five attacks of abdominal pain with the specific characteristics mentioned above, with no evidence of other gastrointestinal disease.
Treatment and Management
- Acute Treatment: During an attack, sleep is often the most effective remedy. Doctors may prescribe NSAIDs (like ibuprofen) or triptans (migraine-specific medication) if caught early.
- Prevention: Maintaining a regular schedule for meals and sleep is vital.
- Natural Approaches: Avoiding known food triggers (using an elimination diet) and managing stress through relaxation techniques are the cornerstones of preventing abdominal migraines. Magnesium supplements are also frequently used as a preventative natural remedy.
Conclusion
Abdominal pain is a complex medical presentation that acts as a window into the body’s internal state. From the fleeting discomfort of a heavy meal to the acute emergency of a ruptured appendix, the abdomen tells a story. By understanding the anatomy, the types of pain, and the potential causes, individuals are better equipped to seek timely medical help when necessary.
While the internet can provide information, it cannot replace a physical examination. If you are in doubt about abdominal pain, err on the side of caution. The abdomen is the core of our physical being—treating it with care, listening to its signals, and maintaining digestive health are essential components of overall well-being. Always consult a healthcare provider for persistent or severe symptoms, as early intervention is the key to successful outcomes in the vast majority of abdominal pathologies.
The Healing Power of Nature and Habit: Managing Abdominal Pain
While medical intervention is critical for acute and severe conditions (like appendicitis or aneurysms), a significant portion of abdominal pain—particularly chronic and functional pain—can be managed, prevented, or alleviated through natural remedies and lifestyle modifications. The gut is highly responsive to what we consume, how we move, and even how we think. Below is a breakdown of how natural approaches can address the specific types of pain mentioned in the guide.
Dietary Interventions and Natural Remedies
For Gas, Bloating, and Indigestion
- Ginger: Perhaps the most studied natural remedy for nausea and digestion. Ginger contains compounds called gingerols and shogaols that help speed up stomach emptying. This is particularly effective for the “fullness” and epigastric pain associated with indigestion.
- Peppermint Oil: Peppermint is a natural antispasmodic. It contains menthol, which relaxes the smooth muscles of the intestines. Enteric-coated peppermint oil capsules are widely used to reduce the cramping and sharp pains associated with IBS and trapped gas.
- Fennel Seeds: Traditionally used in many cultures after meals, fennel seeds help relax the digestive muscles and reduce gas. Chewing a teaspoon of seeds or drinking fennel tea can alleviate lower abdominal bloating.
For Gastritis, GERD, and Peptic Ulcers
- Licorice Root (DGL): Deglycyrrhizinated licorice (DGL) is a specific form of licorice that coats the stomach lining, protecting it from acid. It can be an effective natural supplement for healing the burning pain of gastritis and ulcers, unlike standard NSAIDs, which can worsen these conditions.
- Slippery Elm: This herb creates a mucilage (a thick, sticky substance) when mixed with water, which coats and soothes the inflamed mucous membranes of the esophagus and stomach, providing relief from the burning pain of GERD.
- Apple Cider Vinegar (ACV): While counterintuitive, some cases of heartburn are caused by low stomach acid rather than high acid. A teaspoon of ACV in water can help balance stomach pH and improve digestion, reducing epigastric pressure.
For Inflammatory Bowel Disease (IBD) and Diverticulitis
- Turmeric (Curcumin): Turmeric is a potent anti-inflammatory. Studies suggest that curcumin supplements can help maintain remission in Ulcerative Colitis and Crohn’s disease by reducing the inflammatory markers that cause abdominal pain and cramping.
- Probiotics: Maintaining a healthy gut microbiome is essential. For conditions like IBS and post-diverticulitis recovery, high-quality probiotics can restore balance to the gut flora, reducing gas production and improving bowel regularity.
For Kidney Stones and Urinary Issues
- Hydration: The most effective natural “remedy” for kidney stones is water. Increasing fluid intake helps flush the kidneys and can aid in passing smaller stones. It also dilutes urine to prevent new stone formation.
- Dandelion Root: Often used as a diuretic, dandelion root tea can help increase urine production, potentially helping to flush out the urinary tract and prevent kidney stone formation.
Lifestyle Modifications
The Low-FODMAP Diet for IBS One of the most effective lifestyle changes for chronic lower abdominal pain and IBS is the Low-FODMAP diet. FODMAPs are short-chain carbohydrates (fermentable oligosaccharides, disaccharides, monosaccharides, and polyols) that are poorly absorbed in the small intestine. They draw water into the intestine and ferment in the colon, causing gas and pain. Reducing foods like onions, garlic, wheat, and certain fruits can dramatically reduce IBS pain.
Stress Management for Functional Pain. The “Gut-Brain Axis” is a real physiological connection. Stress triggers the release of cortisol and adrenaline, which can disrupt digestion, causing spasms in the colon (visceral hypersensitivity).
- Mindfulness and Meditation: Reducing the stress response can physically relax the digestive tract.
- Cognitive Behavioral Therapy (CBT): CBT has shown remarkable success in treating chronic abdominal pain by helping patients manage the psychological distress that amplifies physical pain signals.
Eating Habits for GERD and Gastritis
- Portion Control: Overeating expands the stomach, pushing acid up into the esophagus. Eating smaller, more frequent meals prevents the “epigastric pressure” common in GERD.
- Meal Timing: Eating late at night and lying down shortly after is a primary cause of nocturnal abdominal pain. A lifestyle change of finishing meals at least 3 hours before bed allows the stomach to empty before sleep.
Physical Movement for Constipation and Gas
- Yoga Poses: Specific poses like “Apanasana” (knees-to-chest) or “Cat-Cow” physically massage the abdominal organs and encourage the movement of gas and stool through the intestines.
- Walking: A simple 15-minute walk after a meal stimulates gastric motility (the movement of food through the digestive tract), reducing the risk of bloating and cramping.
Heat Therapy: Applying a heating pad to the lower abdomen is a time-honored remedy. Heat increases blood flow to the area and relaxes the smooth muscles, which is particularly effective for menstrual cramps (dysmenorrhea) and intestinal spasms.
FAQs
General Symptoms & Causes
- Why does my stomach hurt more when I am stressed?
Stress activates the “fight or flight” response, which diverts blood away from the digestive system. This can cause spasms, increase pain sensitivity (visceral hypersensitivity), and disrupt the balance of gut bacteria, leading to cramping or nausea.
- How can I tell the difference between gas pain and appendicitis?
Gas pain usually feels like a sharp, stabbing sensation that moves around the abdomen and is often relieved by passing gas or belching. Appendicitis pain typically starts near the navel and migrates to the lower right side, where it becomes constant, severe, and tender to the touch.
- What does “rebound tenderness” mean?
Rebound tenderness is pain that occurs when pressure is applied to the abdomen and is quickly released. It is a classic sign of peritonitis (inflammation of the abdominal lining) and suggests a serious condition like a ruptured appendix or diverticulitis.
- Can dehydration cause abdominal pain?
Yes. Dehydration can lead to constipation, which causes cramping and lower abdominal pain. In severe cases, it can contribute to kidney stones, which cause excruciating flank and abdominal pain.
- Why do I have abdominal pain only after eating?
Pain after eating is often linked to the digestive organs. It could be Gallbladder pain (specifically after fatty meals), Gastritis (due to acid production), or IBS (due to the gastrocolic reflex triggering cramps).
Diagnosis & Medical Tests
- Is a CT scan always necessary for stomach pain?
No. Doctors usually order a CT scan if the physical exam suggests a surgical issue (like appendicitis or blockage) or if the diagnosis is unclear. For mild, chronic pain, an ultrasound or endoscopy might be preferred.
- What is the difference between IBS and IBD?
IBS (Irritable Bowel Syndrome) is a functional disorder; the gut looks normal but doesn’t work properly, causing cramps and altered habits. IBD (Inflammatory Bowel Disease) is a structural disease where there is visible inflammation and damage to the intestinal lining (like Crohn’s or Ulcerative Colitis).
- Can a blood test detect stomach pain causes?
A blood test cannot “see” pain, but it can detect signs of infection (high white blood cell count), inflammation (CRP or ESR levels), or organ dysfunction (liver enzymes for gallbladder/liver issues).
- Why do doctors press on my stomach during an exam?
They are checking for tenderness, guarding (muscle tensing), masses, or enlarged organs. This helps them localize the pain to a specific quadrant.
- What is a “surgical abdomen”?
This is a term for severe abdominal pain that requires immediate surgery, such as a ruptured appendix, a perforated ulcer, or an ectopic pregnancy.
Natural Remedies & Home Care
- Is ginger actually effective for stomach aches?
Yes. Clinical studies suggest ginger is effective for nausea and can help speed up gastric emptying, which relieves the feeling of fullness and bloating.
- Should I use heat or ice for abdominal pain?
Heat (like a heating pad) is generally better for muscle cramps, menstrual pain, and gas, as it relaxes the muscles. Ice is rarely used for internal abdominal pain unless there is acute inflammation that needs numbing, but heat is the standard home remedy.
- Does peppermint tea help with bloating?
Yes. Peppermint contains menthol, which acts as an antispasmodic, relaxing the smooth muscles of the intestines and allowing trapped gas to pass.
- What is the BRAT diet?
BRAT stands for Bananas, Rice, Applesauce, and Toast. It is a bland diet often recommended for gastroenteritis or stomach viruses because these foods are easy to digest and help firm up stool.
- Can probiotics stop stomach pain?
Probiotics can help over time by balancing the gut microbiome. They are particularly useful for preventing bloating and pain associated with IBS or after taking antibiotics, but they are not an instant painkiller.
Specific Conditions
- What does gallbladder pain feel like?
Gallbladder pain (biliary colic) is usually a severe, steady ache in the right upper quadrant or epigastric region. It often radiates to the right shoulder blade and can be accompanied by nausea and vomiting.
- Can constipation cause severe pain?
Absolutely. A fecal impaction or severe constipation can cause cramping that mimics appendicitis or kidney stones. It typically presents as diffuse or lower left quadrant pain.
- What is the “referred pain” of a heart attack?
During a heart attack (specifically inferior myocardial infarction), pain is often felt in the epigastric region (upper middle abdomen) rather than the chest. It can mimic severe indigestion.
- What are the symptoms of an ovarian cyst rupture?
A rupture usually causes sudden, sharp, severe pain on one side of the lower abdomen. It may be accompanied by light vaginal spotting or dizziness.
- Is appendicitis always an emergency?
Yes. If left untreated, the appendix can burst, spreading infection throughout the abdomen (peritonitis), which is life-threatening.
Lifestyle & Diet
- What foods trigger IBS pain?
Common triggers include high-FODMAP foods such as onions, garlic, beans, wheat, dairy products (lactose), and certain fruits like apples and watermelon.
- Does drinking water help gastritis?
Yes. Water helps dilute stomach acid and keeps the mucous lining hydrated. However, drinking large amounts during meals can sometimes bloat the stomach; it is better to sip water throughout the day.
- How does sleep affect abdominal pain?
Poor sleep can increase inflammation and pain sensitivity. Additionally, lying flat can worsen GERD pain, so elevating the head while sleeping is a necessary lifestyle change for those with acid reflux.
- Can exercise hurt my stomach?
Intense exercise right after eating can cause “runner’s stitch” or cramping. However, regular, moderate exercise like walking or yoga improves gut motility and reduces chronic constipation and gas.
- Why does alcohol cause abdominal pain?
Alcohol irritates the stomach lining (gastritis), increases acid production, and can inflame the pancreas (pancreatitis). It is a major trigger for upper abdominal pain.
Prevention & Red Flags
- How can I prevent kidney stones naturally?
The most effective prevention is drinking enough water to produce 2 to 2.5 liters of urine daily. Reducing salt and animal protein intake also helps prevent stone formation.
- When should I stop self-treating and see a doctor?
You should see a doctor if the pain is severe, lasts more than a few days, is accompanied by fever, inability to pass stool, blood in stool/vomit, or if the abdomen feels rigid and hard.
- Is it true that I shouldn’t eat if my stomach hurts?
If you have acute vomiting or severe pain, resting the stomach (NPO – nothing by mouth) for a few hours is often advised. However, for chronic issues like ulcers, eating small, bland meals is important to buffer stomach acid.
- Can smoking cause stomach pain?
Yes. Smoking increases stomach acid, weakens the valve between the stomach and esophagus (worsening GERD), and is a major risk factor for Crohn’s disease and ulcers.
- Are herbal remedies safe for everyone?
No. “Natural” does not mean safe. For example, licorice root can raise blood pressure, and some herbs interact with blood thinners. Always consult a doctor before starting herbal supplements, especially if you are on other medications.
- Can children get “migraines” in their stomachs?
Yes, this is known as an abdominal migraine. It causes severe pain around the belly button, nausea, and vomiting, often without a headache. It is a real medical condition and not just “attention-seeking” behavior.
- How is an abdominal migraine different from a stomach virus?
While both cause vomiting and pain, a stomach virus usually includes diarrhea and fever, and lasts a few days. An abdominal migraine typically has no fever or diarrhea, follows specific triggers (like stress or foods), and the child is usually completely symptom-free between attacks.
Disclaimer: The content on this blog is for informational purposes only. and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. The author’s opinions are personal and not endorsed. Efforts are made to provide accurate information, but completeness, accuracy, or reliability are not guaranteed. The author is not liable for any loss or damage resulting from the use of this blog. It is recommended to use the information on this blog at your own discretion.