Table of Contents
The Spinning World: A Comprehensive Guide to Understanding, Diagnosing, and Treating Vertigo
Introduction: When the World Won’t Stand Still
Imagine waking up in the middle of the night to use the bathroom. You swing your legs out of bed, plant your feet on the floor, and suddenly, the room violently tilts to the left. You grab the mattress, your heart hammering against your ribs, convinced you are about to fall into an abyss. You close your eyes tight, willing the sensation to stop, but the spinning persists. You feel nauseous, disoriented, and terrified. You haven’t moved, yet the world is reeling around you.
This is the reality for millions of people worldwide who suffer from vertigo. It is a sensation that strips away your sense of stability, making the simplest tasks—walking down a hallway, driving a car, or even turning your head to look at a loved one—feel like a Herculean challenge. Vertigo is more than just dizziness; it is a profound disruption of the body’s equilibrium system, a glitch in the complex hardware that allows us to navigate gravity.
In the medical community, vertigo is often a puzzle that requires detective work to solve. Is it a problem in the ear? A glitch in the brain? A reaction to medication? The causes are myriad, and the symptoms can be debilitating. However, despite its frightening presentation, vertigo is often manageable. With the right diagnosis and treatment, the spinning can stop, and balance can be restored.
This comprehensive guide aims to demystify vertigo. We will journey through the intricate anatomy of the inner ear, explore the various pathologies that trigger the spin, detail the diagnostic maze patients often navigate, and outline the cutting-edge treatments available today. Whether you are a sufferer seeking answers or a caregiver looking for understanding, this is your roadmap to a steady world.
Is Vertigo a Disease? The Semantics of Spinning
One of the most common misconceptions is that vertigo is a disease. It is crucial to clarify this distinction immediately. Vertigo is not a disease; it is a symptom.
Think of vertigo like a fever. A fever is not a disease itself; it is a signal that the body is fighting an infection, reacting to a drug, or suffering from inflammation. Similarly, vertigo is a signal—a specific type of dizziness—that indicates a dysfunction somewhere in the body’s balance system.
The Definition Clinically, vertigo is defined as the false sensation that you or your surroundings are moving. It is distinct from lightheadedness (presyncope), disequilibrium (a sense of imbalance without spinning), and anxiety-related “dizziness.” Vertigo implies a rotational component—”the room is spinning” or “I am spinning.”
Because it is a symptom, a diagnosis of “vertigo” is just the starting point. The critical medical question is: What is causing the vertigo? The answer could range from loose calcium crystals in the ear to a tumor pressing on a nerve. Treating the vertigo requires identifying and addressing the underlying etiology.
The Anatomy of Balance – How We Stay Upright
To understand why vertigo happens, we must first understand how balance works. Balance is not just a matter of strong legs; it is a complex neurological calculation performed by the brain.
The body maintains equilibrium through a triad of systems, often called the Balance Triad:
- The Visual System (Eyes): Your eyes tell your brain where you are in space relative to gravity. You see the horizon; you see the walls.
- The Somatosensory System (Proprioception): Nerves in your skin, muscles, and joints tell your brain where your body parts are. You feel the floor under your feet; you sense the position of your head.
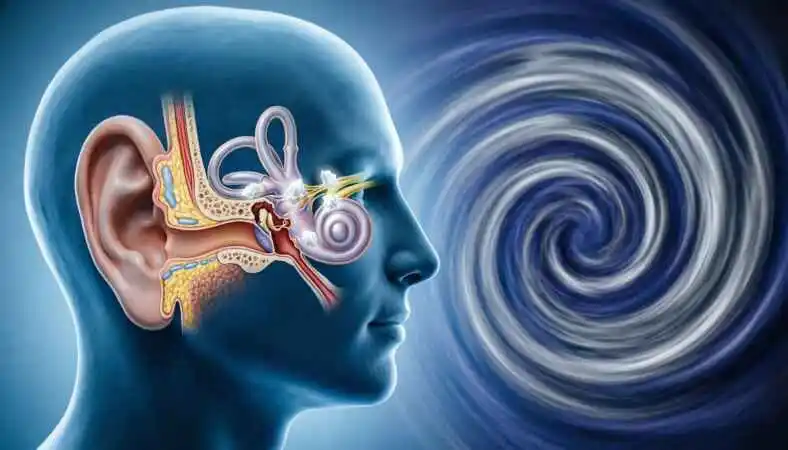
- The Vestibular System (Inner Ear): This is the master compass. Located deep within the temporal bone of the skull, the vestibular system detects motion and gravity independent of vision.
The Vestibular Apparatus Inside each ear, we have a structure called the labyrinth. It consists of two main parts:
- The Cochlea: For hearing.
- The Vestibular System: For balance.
The vestibular system includes three semicircular canals (arranged at right angles to detect rotational movement) and two otolith organs (the utricle and saccule) which detect linear acceleration and head position. These structures are filled with fluid (endolymph) and lined with hair cells that act as sensors.
When you turn your head to the right, the fluid in your right ear lags, pushing on the hair cells. This sends an electrical signal to the brain saying, “We are turning right.” Simultaneously, the signal from the left ear decreases. The brain compares the input from both ears. If they match, you perceive smooth movement. If there is a mismatch—if one ear signals “spinning” while the other signals “stillness”—the brain creates the sensation of vertigo.
The Many Faces of Vertigo – Causes and Risk Factors
Vertigo is broadly categorized into two types based on the location of the problem: Peripheral Vertigo (originating in the inner ear) and Central Vertigo (originating in the brain). Peripheral causes are far more common, accounting for roughly 80% of cases.
Peripheral Causes (The Inner Ear)
- Benign Paroxysmal Positional Vertigo (BPPV) This is the single most common cause of vertigo. The name is descriptive:
- Benign: It isn’t life-threatening.
- Paroxysmal: It comes in sudden, brief spells.
- Positional: It is triggered by changes in head position.
- Vertigo: It causes spinning.
- The Mechanism: Inside the utricle, calcium carbonate crystals (otoconia) are normally embedded in a gel. Due to age, head trauma, or infection, these crystals can dislodge and migrate into one of the semicircular canals. When you move your head (like rolling over in bed or looking up), these loose crystals shift, creating a “plunger” effect on the fluid. This sends a false signal to the brain that the head is spinning violently.
- Symptoms: Short bursts of spinning (less than a minute) triggered by specific movements.
- Meniere’s Disease This is a chronic, progressive condition caused by an abnormal buildup of fluid (endolymph) in the inner ear.
- The Mechanism: The increased pressure stretches the membranes of the labyrinth, affecting both hearing and balance.
- Symptoms: The hallmark of Meniere’s is a triad of symptoms: episodic vertigo (lasting 20 minutes to several hours), fluctuating hearing loss, and tinnitus (ringing in the ear). Patients often report a feeling of “fullness” or pressure in the affected ear before an attack.
- Vestibular Neuritis and Labyrinthitis These conditions involve inflammation, usually viral in origin.
- Vestibular Neuritis: Inflammation of the vestibular nerve. It causes severe, constant vertigo, nausea, and vomiting that can last for days. Hearing remains normal.
- Labyrinthitis: Inflammation of the entire labyrinth. It presents with the same severe vertigo but also includes hearing loss.
- Cause: Often follows a viral infection like the flu or a cold. It can be debilitating initially but usually resolves as the inflammation subsides and the brain compensates.
- Vestibular Schwannoma (Acoustic Neuroma) A benign tumor that grows on the vestibular nerve. It usually grows slowly and causes gradual hearing loss and mild imbalance rather than sudden, violent vertigo.
Central Causes (The Brain)
Central vertigo is less common but implies a more serious pathology in the brainstem or cerebellum.
- Stroke or Transient Ischemic Attack (TIA) A stroke affecting the cerebellum or the brainstem can cause vertigo. This is a medical emergency.
- Red Flags: Vertigo accompanied by double vision, slurred speech, difficulty swallowing, limb weakness, or numbness.
- Migraine Vestibular migraine is a leading cause of vertigo, particularly in younger people. The vertigo may occur with or without the headache phase. It can be triggered by stress, specific foods, or hormonal changes.
- Multiple Sclerosis (MS) MS damages the myelin sheath covering nerves. If this damage occurs in the brainstem, it can disrupt balance signals.
- Medication Toxicity Certain medications, particularly aminoglycoside antibiotics (like gentamicin), are ototoxic (toxic to the ear) and can cause permanent damage to the vestibular system.
The Symptom Profile – Recognizing the Signs
While the primary symptom is the sensation of movement, vertigo is rarely an isolated event. It brings a host of associated symptoms that help doctors pinpoint the cause.
- Nystagmus: This is the most objective sign. It is an involuntary, rapid movement of the eyes. In peripheral vertigo, the eyes usually beat in one direction (horizontal-torsional). In central vertigo, the pattern can be chaotic or vertical. A doctor can use special goggles (Frenzel lenses) to see this clearly.
- Nausea and Vomiting: The conflict between what the eyes see and what the inner ear feels stimulates the vagus nerve and the area postrema (the vomiting center) in the brain.
- Hearing Changes: Loss of hearing or ringing (tinnitus) suggests Meniere’s disease or labyrinthitis.
- Visual Disturbances: Oscillopsia is the sensation that the visual world is bouncing or “jiggling” as you walk.
- Anxiety: There is a strong link between vertigo and anxiety. The sensation of losing control is terrifying, and the fear of an attack can lead to agoraphobia (fear of leaving safe spaces).
Diagnosis – The Medical Detective Work
Diagnosing vertigo is like solving a puzzle. The doctor relies heavily on the patient’s history, as the physical exam is often normal between attacks.
- The Clinical History The doctor will ask:
- Does the room spin, or do you feel lightheaded?
- How long do the attacks last? (Seconds? Minutes? Hours? Days?)
- What triggers it? (Lying down? Stress? Coughing?)
- Do you have hearing loss or ringing?
- Physical Examination
- The Dix-Hallpike Maneuver: The gold standard test for BPPV. The patient sits on the exam table and is quickly lowered back with the head turned to one side. If the patient has loose crystals in the posterior canal, this movement will trigger vertigo and a characteristic eye twitch (nystagmus) after a short delay.
- Head Impulse Test: The doctor turns the patient’s head rapidly to the side. If the eyes cannot stay focused on the doctor’s nose (and make a “catch-up” saccade), it suggests a weak vestibular nerve on that side.
- Audiometry A hearing test is essential if the patient reports hearing loss. It can distinguish between nerve hearing loss (sensorineural) and conductive loss.
- Imaging
- MRI: Magnetic Resonance Imaging is used to rule out central causes like tumors or stroke. It provides detailed images of the brainstem and cerebellum.
- CT Scan: Computed Tomography is used to look at bone structure, such as the temporal bone, if a structural abnormality is suspected.
- Vestibular Testing
- VNG (Videonystagmography): Goggles record eye movements while the patient performs various tasks.
- Rotary Chair Testing: The patient sits in a rotating chair while eye movements are recorded. This assesses how well the vestibular system is functioning.
Treatment – Stopping the Spin
Treatment depends entirely on the underlying cause.
Treating BPPV
(Benign Paroxysmal Positional Vertigo) refers to the specific physical methods used to move loose calcium crystals out of the semicircular canals in your inner ear.
The treatment for BPPV is mechanical, not pharmaceutical.
- The Epley Maneuver (Canalith Repositioning): This is a series of specific head movements designed to guide the loose crystals out of the semicircular canal and back into the utricle, where they can dissolve or be reabsorbed. It has a high success rate (about 80-90%) and can be done in a doctor’s office in minutes.
- Semont Maneuver: An alternative repositioning technique.
Treating Meniere’s Disease :
This is a chronic, progressive disorder of the inner ear caused by an abnormal buildup of fluid (endolymph) within the labyrinth. This increased pressure disrupts both hearing and balance signals.
There is no cure for Meniere’s, but symptoms can be managed.
- Dietary Changes: A low-sodium diet is crucial to reduce fluid retention in the inner ear. Avoiding caffeine and alcohol also helps.
- Diuretics: Medications that help the body excrete excess fluid.
- Injections: In severe cases, injections of gentamicin (to chemically ablate the balance function in that ear) or steroids (to reduce inflammation) are used.
- Surgery: Endolymphatic sac decompression or vestibular nerve section may be considered in refractory cases.
Treating Vestibular Neuritis
- Vestibular Suppressants: Medications like meclizine or diazepam are used for the first few days to suppress the acute nausea and spinning.
- Steroids: High-dose corticosteroids may reduce inflammation and improve long-term outcomes.
- Vestibular Rehabilitation Therapy (VRT): This is the most important long-term treatment. If the nerve is damaged, the brain must learn to rely on the other ear and the eyes to balance. VRT involves specific exercises to promote “central compensation.”
Treating Central Vertigo
- Stroke: Immediate emergency care (tPA or thrombectomy).
- Migraine: Migraine prophylaxis (beta-blockers, topiramate) and lifestyle changes.
Natural Remedies and Lifestyle Adjustments
While medical intervention is necessary for acute conditions, lifestyle plays a massive role in managing chronic dizziness.
- Hydration Dehydration can thicken the blood and alter the pressure in the inner ear. Drinking adequate water is a simple yet effective preventative measure.
- Sleep Hygiene Fatigue exacerbates vestibular symptoms. A regular sleep schedule helps the brain recalibrate.
- Stress Management Stress increases cortisol and adrenaline, which can disrupt the vestibular system. Yoga, meditation, and deep breathing exercises are beneficial.
- Ginger Ginger has natural anti-nausea properties. Many vertigo sufferers find that ginger tea or supplements help settle the stomach during an attack.
- Ginkgo Biloba Some studies suggest Ginkgo Biloba may improve blood flow to the brain and inner ear, potentially helping with chronic dizziness, though evidence is mixed.
- Safety Modifications For those with chronic balance issues, preventing falls is paramount.
- Install grab bars in the bathroom.
- Remove loose rugs.
- Use nightlights to aid visual compensation in the dark.
The Psychological Impact – The Invisible Burden
We cannot discuss vertigo without acknowledging its psychological toll. Because the symptom is invisible—others cannot see the room spinning—patients often feel misunderstood or dismissed. The unpredictability of attacks leads to constant vigilance and fear.
Vestibular Anxiety: The fear of falling or becoming incapacitated in public can lead to social isolation. This anxiety creates a vicious cycle: anxiety heightens the body’s sensitivity to imbalance, which triggers more vertigo, which fuels more anxiety. Treating the anxiety (through CBT or medication) is often a necessary component of treating the vertigo.
Prevention – Protecting Your Balance
While you cannot prevent all causes of vertigo (like a viral infection), you can protect your vestibular health.
- Protect your head: Wear helmets during biking or skiing to prevent trauma that dislodges crystals.
- Manage Cardiovascular Health: High blood pressure, diabetes, and high cholesterol damage the tiny blood vessels supplying the inner ear. A heart-healthy diet is an ear-healthy diet.
- Avoid Ototoxicity: Be aware of the side effects of medications. If you are prescribed aminoglycoside antibiotics, discuss monitoring with your doctor.
Natural Remedies and Lifestyle Modifications for Vertigo Management
While medical interventions like the Epley maneuver or prescription medications are often necessary for acute episodes, the long-term management of vertigo heavily relies on lifestyle adjustments and natural supportive therapies. These approaches aim to reduce the frequency of attacks, lessen the severity of symptoms, and help the brain compensate for inner ear imbalances.
- The Role of Hydration and Electrolytes
Dehydration is a silent trigger for vertigo. The inner ear fluid (endolymph) relies on a precise balance of water and electrolytes to function correctly.
- The Mechanism: When the body is dehydrated, blood volume decreases, reducing blood flow to the brain and altering the chemical composition of the inner ear fluids. This can trigger dizziness or exacerbate conditions like BPPV.
- The Strategy: Aim for at least 8 glasses of water daily. If you are active or live in a hot climate, increase this amount.
- Electrolyte Balance: Potassium and magnesium are critical for nerve signal transmission. Low levels can disrupt vestibular signaling.
- Natural Sources: Bananas, avocados, spinach (potassium); almonds, pumpkin seeds, dark chocolate (magnesium).
- Dietary Interventions: The Low-Sodium and Migraine Diet
For conditions like Meniere’s Disease and Vestibular Migraine, diet is often the first line of defense.
- Sodium Restriction (For Meniere’s):
- Goal: Reduce fluid retention in the inner ear. Excess sodium causes the body to retain water, which increases pressure in the endolymphatic sac.
- Target: Ideally, keeping sodium intake under 1,500mg to 2,000mg per day.
- Action: Eliminate the “Salty Six”: breads/rolls, pizza, sandwiches, cold cuts/cured meats, soups, and burritos/tacos. Avoid adding salt at the table.
- Trigger Avoidance (For Vestibular Migraine):
- Tyramine: An amino acid found in aged cheeses, cured meats, and fermented foods (soy sauce, sauerkraut) that can trigger migraines.
- Caffeine and Alcohol: These substances alter blood flow and can dehydrate the body. Caffeine can sometimes help in small amounts (constricting blood vessels), but withdrawal or overconsumption often triggers vertigo.
- MSG (Monosodium Glutamate): A flavor enhancer found in processed foods and Chinese takeout that acts as an excitotoxin and can overstimulate the nervous system.
- Herbal and Natural Supplements
While supplements should not replace medical treatment, several have shown promise in managing vertigo symptoms.
- Ginger (Zingiber officinale):
- How it works: Ginger contains compounds called gingerols and shogaols, which have potent anti-emetic (anti-nausea) properties. It acts on the digestive system and the central nervous system to calm nausea caused by motion sickness and vertigo.
- Usage: Ginger tea, chewable ginger chews, or 250mg capsules. It is most effective when taken at the onset of symptoms.
- Ginkgo Biloba:
- How it works: Ginkgo is known for improving blood flow, particularly microcirculation in the brain and inner ear. Some studies suggest it can be as effective as betahistine (a common vertigo drug) for vestibular dysfunction.
- Caution: Ginkgo thins the blood and should not be taken by individuals on blood thinners like Warfarin or aspirin.
- Vitamin D and Calcium:
- The Connection: Research indicates a strong link between Vitamin D deficiency and Benign Paroxysmal Positional Vertigo (BPPV). The otoconia (crystals) in the ear are made of calcium carbonate. Vitamin D helps regulate calcium metabolism.
- The Evidence: Patients with recurrent BPPV who correct low Vitamin D levels often experience a significant reduction in recurrence rates.
- Butcher’s Broom:
- Often used in Europe for orthostatic hypotension (dizziness upon standing), this herb helps improve venous circulation, preventing blood from pooling in the legs and ensuring adequate blood flow to the brain.
- Physical Therapy and Home Exercises
Beyond the Epley Maneuver, specific exercises can retrain the brain to handle conflicting signals.
- Vestibular Rehabilitation Therapy (VRT):
- This is a specialized form of therapy designed to promote central compensation. If one ear is weak, the brain learns to rely more heavily on the other ear and visual cues.
- Gaze Stabilization Exercises (VOR x1): Focus on a small letter on a wall. Move your head side to side while keeping your eyes locked on the target. Do this for 30-60 seconds. This trains the Vestibulo-Ocular Reflex (VOR).
- Brandt-Daroff Exercises:
- Often prescribed for BPPV, these are movements that can be done at home. They involve moving from a sitting position to a lying position on one side, waiting for the dizziness to pass, and then repeating on the other side. This helps disperse loose crystals and habituate the brain to the sensation of movement.
- Sleep Hygiene and Stress Management
The vestibular system is highly sensitive to stress and fatigue.
- The Stress-Vertigo Loop: Stress releases cortisol and adrenaline, which can disrupt the delicate fluid balance in the inner ear and heighten the brain’s sensitivity to motion signals. Anxiety often leads to hyperventilation, which changes CO2 levels in the blood and causes lightheadedness.
- Deep Breathing Techniques: Diaphragmatic breathing activates the parasympathetic nervous system (the “rest and digest” system), helping to lower heart rate and stabilize blood pressure during a dizzy spell.
- Sleep Position:
- For BPPV sufferers, sleeping with the head slightly elevated (using two pillows) can prevent crystals from shifting into the semicircular canals during the night.
- Avoid sleeping on the “bad side” (the ear affected by the vertigo).
- Proprioceptive Training
Since the balance triad relies on the eyes, ears, and proprioception (body awareness), strengthening the proprioceptive system can compensate for inner ear weakness.
- Tai Chi and Yoga: These practices focus on slow, deliberate movements, weight shifting, and grounding. They improve the connection between the brain and the muscles/joints, providing a “safety net” for balance. Tai Chi has been extensively studied for fall prevention in the elderly and those with vestibular deficits.
- Barefoot Walking: Walking barefoot on safe surfaces (grass, sand, carpet) stimulates the nerves in the soles of the feet, enhancing proprioceptive feedback to the brain.
- Environmental Modifications
While not a “treatment,” modifying the environment is a crucial lifestyle adjustment for preventing falls and reducing sensory overload.
- Lighting: Keep hallways and bathrooms well-lit at night. In darkness, the brain loses visual input and relies entirely on the compromised vestibular system, increasing fall risk. Use motion-sensor nightlights.
- Contrast: Ensure high contrast between floors and walls. Low-contrast environments (white walls, beige carpet) can cause visual confusion for those with vestibular issues.
- Reduce Screen Time: Excessive scrolling on phones or watching fast-moving videos can trigger “digital vertigo” or cybersickness due to a mismatch between visual motion and physical stillness. Taking frequent breaks using the 20-20-20 rule (every 20 minutes, look 20 feet away for 20 seconds) helps.
Conclusion: Finding Solid Ground
Vertigo is a thief. It steals moments, confidence, and stability. But it is not invincible. In the vast majority of cases, the spinning can be stopped. Whether it’s a simple head maneuver to relocate a loose crystal, a diuretic to manage fluid pressure, or dedicated physical therapy to retrain the brain, solutions exist.
If you or a loved one experiences vertigo, do not resign yourself to a life of dizziness. Seek a specialist—an otolaryngologist (ENT) or a neurologist—who specializes in vestibular disorders. Be an advocate for your health. Keep a diary of your symptoms. Understand that while the spinning feels endless, it is merely a symptom signaling a specific, solvable problem.
The world may spin, but with the right knowledge and care, you can find your footing once again.
FAQS
Basics and Definition
- Is vertigo a disease?
No, vertigo is not a disease itself; it is a symptom of an underlying issue, usually related to the inner ear or brain.
- How is vertigo different from general dizziness?
Vertigo is specifically the false sensation that you or your surroundings are spinning, whereas dizziness is a broader term that can include lightheadedness, unsteadiness, or feeling faint.
- What is the “Balance Triad”?
The Balance Triad refers to the three systems the body uses to stay upright: the visual system (eyes), the somatosensory system (proprioception in muscles/joints), and the vestibular system (inner ear).
- What is the function of the vestibular system?
The vestibular system, located in the inner ear, detects motion and gravity, acting as the body’s “master compass” to help the brain understand head position and movement.
Causes and Types
- What is the most common cause of vertigo?
Benign Paroxysmal Positional Vertigo (BPPV) is the most common cause. It occurs when loose calcium crystals migrate into the semicircular canals of the inner ear.
- What triggers BPPV?
BPPV is triggered by changes in head position, such as rolling over in bed, looking up, or bending over.
- What are the hallmark symptoms of Meniere’s Disease?
Meniere’s Disease is characterized by a triad of symptoms: episodic vertigo, fluctuating hearing loss, and tinnitus (ringing in the ears), often accompanied by a feeling of fullness in the ear.
- What is the difference between Vestibular Neuritis and Labyrinthitis?
Both are caused by inflammation (often viral). Vestibular Neuritis affects the balance nerve and causes vertigo, but preserves hearing. Labyrinthitis affects the entire inner ear, causing vertigo and hearing loss.
- What is Central Vertigo?
Central vertigo originates from a problem in the brain (specifically the brainstem or cerebellum), such as a stroke, migraine, or tumor, rather than the inner ear.
- Can medications cause vertigo?
Yes, certain medications, particularly aminoglycoside antibiotics, can be ototoxic (toxic to the ear) and cause permanent damage to the vestibular system, leading to vertigo.
Symptoms and Diagnosis
- What is nystagmus?
Nystagmus is an involuntary, rapid movement of the eyes. It is a key objective sign that doctors look for when diagnosing vertigo.
- Why does vertigo often cause nausea and vomiting?
The conflicting signals between the eyes and the inner ear confuse the brain, stimulating the vagus nerve and the brain’s vomiting center.
- What is the Dix-Hallpike Maneuver?
It is a diagnostic test used to confirm BPPV. The doctor lowers the patient quickly backward with the head turned to one side to see if it triggers vertigo and nystagmus.
- When is an MRI necessary for vertigo?
An MRI is typically ordered to rule out central causes like stroke, tumors, or multiple sclerosis, especially if the patient has neurological symptoms like slurred speech or double vision.
Medical Treatments
- How is BPPV treated?
The primary treatment is the Epley Maneuver (Canalith Repositioning), a series of specific head movements that guide the loose crystals out of the semicircular canals.
- What is Vestibular Rehabilitation Therapy (VRT)?
VRT is a specialized form of physical therapy that retrains the brain to compensate for inner ear deficits using specific exercises to improve balance and gaze stability.
- Can Meniere’s Disease be cured?
There is no cure, but it can be managed through a low-sodium diet, diuretics, and in severe cases, injections or surgery.
- What are VOR exercises?
Vestibulo-Ocular Reflex (VOR) exercises involve focusing on a stationary target while moving the head, helping to stabilize vision during movement.
Natural Remedies and Supplements
- How does ginger help with vertigo?
Ginger has natural antiemetic properties that can calm nausea and settle the stomach during a vertigo attack.
- Can Ginkgo Biloba help with vertigo?
Some studies suggest Ginkgo Biloba may improve blood flow to the brain and inner ear, potentially helping with chronic dizziness, though it should not be used by those on blood thinners.
- Why is hydration important for preventing vertigo?
Dehydration reduces blood volume and alters the chemical composition of inner ear fluids, which can trigger dizziness.
- Is there a link between Vitamin D and vertigo?
Yes, research suggests that Vitamin D deficiency is linked to the recurrence of BPPV, as Vitamin D helps regulate the calcium metabolism of the inner ear crystals.
- What is Butcher’s Broom used for?
Butcher’s Broom is an herb often used to improve venous circulation and treat orthostatic hypotension (dizziness upon standing).
Lifestyle and Diet
- Why is a low-sodium diet recommended for vertigo sufferers?
Reducing sodium intake helps prevent fluid retention in the body, which lowers pressure in the inner ear—a crucial factor for managing Meniere’s Disease.
- What is the “Salty Six” to avoid?
The Salty Six refers to common high-sodium foods: breads/rolls, pizza, sandwiches, cold cuts, soups, and burritos/tacos.
- What foods can trigger vestibular migraines?
Foods high in tyramine (aged cheeses, cured meats), MSG, caffeine, and alcohol can trigger migraines that lead to vertigo.
- How does sleep affect vertigo?
Fatigue can exacerbate vestibular symptoms and heighten the brain’s sensitivity to imbalance signals, making adequate sleep essential for management.
- What is the best sleep position for someone with BPPV?
Sleeping with the head slightly elevated (using two pillows) can prevent loose crystals from shifting into the semicircular canals during the night.
- How can Tai Chi help vertigo patients?
Tai Chi improves proprioception (body awareness) and stability, helping the brain rely on other senses to maintain balance when the inner ear is compromised.
- Can screen time trigger vertigo?
Yes, excessive scrolling on phones or watching fast-moving videos can cause “digital vertigo” or cybersickness due to a mismatch between visual motion and physical stillness.
Medical Disclaimer:
The information provided on this website is for general educational and informational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.